Life with EB: Tough, Time-Consuming, and Fraught with Risk
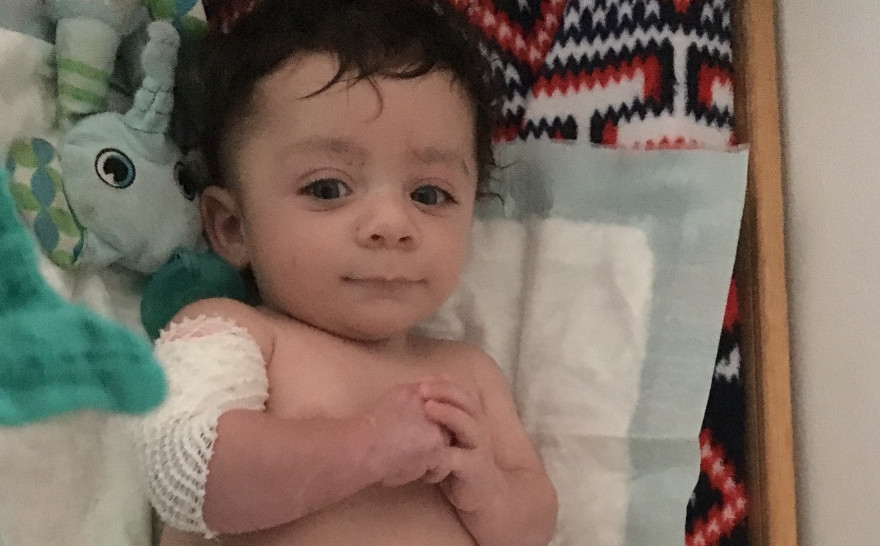
Elijah Dickens, 5 months, was born with epidermolysis bullosa. (Photo courtesy of Jennifer Thompson)
Editor’s note: First of a two-part series on epidermolysis bullosa. The second part, focusing on treatments and care, will follow soon.
For caregivers, epidermolysis bullosa (EB) is complicated, time-consuming, and fraught with risk, something Jennifer Thompson, who has a 5-month-old with EB, learns anew each day.
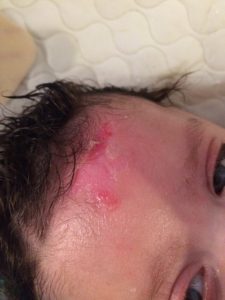
“I put a simple little knit hat on him the other day, didn’t think too much about it, and when I pulled it off, skin came off the side of his face,” said Thompson, 27, of Williamstown, New York. “Anything can happen, and you have to be ready to figure out every situation.”
Thompson’s son, Elijah Dickens, is one of roughly 25,000 people in the U.S. living with EB, a devastating and incurable skin condition caused by the lack of a critical protein that binds skin layers together, according to the Dystrophic Epidermolysis Bullosa Research Association of America, or DEBRA.
Without this protein, the skin tears apart, blisters, and shears off, leading to pain, disfigurement, and sores all over the body, including internally.
For Thompson, life was upended moments after Elijah’s birth, when doctors noticed her baby had skin missing from his arms, legs, and hands. “The doctors called it right away,” she said.
Since then, it’s been a daily struggle figuring out what’s best for a child too young to verbalize where something hurts, while caring for two other young children. Still, there is some semblance of routine. Elijah usually wakes at around 6 a.m. every day, when he has his diaper changed.
“Usually there are blisters, so I pop those,” said Thompson, who lives with her children’s father, a full-time factory worker. “A little later, I change his dressings and pop more blisters. He passes out from crying sometimes. On those days, I take him to the pediatrician.”
Elijah sees a pediatrician a couple of times monthly, and regularly visits an out-of-state dermatologist who specializes in EB.
Thompson is learning techniques to minimize the damage Elijah does to himself. For instance, she liberally applies Aquaphor ointment around his body’s diaper area to act as a barrier when he kicks his legs. Sometimes she’ll add Mepilex Transfer Dressing, used on wounds as a protective layer.
Other general treatments include coconut oil, an antibiotic ointment, and Tylenol and Motrin for pain. Thompson has a morphine spray but doesn’t use it for fear it could harm her baby’s liver. She dresses Elijah in a brand of clothing called Kiki that she orders online and is made for sensitive skin.
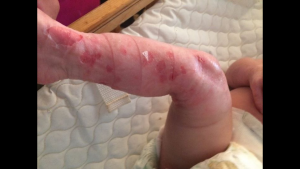 Thompson has considered a bone marrow transplant but wants to first see how more patients fare who have EB simplex, the type of EB Elijah has. Diet-wise, Elijah takes in more calories than normal to compensate for a compromised immune system that makes it harder to gain weight.
Thompson has considered a bone marrow transplant but wants to first see how more patients fare who have EB simplex, the type of EB Elijah has. Diet-wise, Elijah takes in more calories than normal to compensate for a compromised immune system that makes it harder to gain weight.
It all can be overwhelming for Thompson, whose ailing mother helps when she’s able. The family relies on Medicaid, which pays for bandages, antibiotic ointment, and once-weekly nursing care. Followers of her Facebook page, Support Baby Elijah Dickens, also can offer support.
The other children, Thompson said, are adjusting to the extra care their brother needs. “They know he’s not a normal baby. Even teething can cause problems if he puts his hand to his face.”
Like most babies around his age, Elijah likes to scoot on the floor on his tummy. But that is risky because of potential damage to skin on his arms. “I’m always wondering what I should let him do, and whether I should do this, or that. Should I use a cream or what? It’s so hard to know right in the moment,” Thompson said.
Brett Kopelan understands. He’s the father of 9-year-old Rafaella, and has his own stories. Like the time one day when his daughter was acting out.
“We told her, ‘Don’t you know how lucky you are? You have two parents who love you very much.’ She said, ‘I’m not lucky, I have EB.’ But we try to get her to understand that although she does have EB, it’s only a part of her,” said Kopelan, executive director of DEBRA of America, a nonprofit that supports the EB community.
For the most part, Rafaella does understand. “She gets stared at and it used to bother her, but now when it happens she just says hi,” said Kopelan, whose family lives just outside New York City. His wife no longer works so she can help care for their daughter.
But it’s been a long road. Rafaella was born two weeks late, missing skin on both feet and on the back of one hand. “We were told not to worry, that she was probably just overcooked,” Kopelan said. Nine days later Rafaella was diagnosed with the recessive dystrophic form of EB, which involves collagen production.
Hoping for a dramatic improvement in the disease, her parents had her undergo a bone marrow transplant in 2010. While the procedure was considered successful overall, its net outcome is complex.
“Medically she’s doing well, she’s producing protein she didn’t before,” Kopelan said. “On the other hand, she still has a serious case of EB.”
He said the surgery is hard on the patient and the family. “It’s a god-awful procedure. If you think a common cold can kill you because your immune system is knocked out … Transplants are serious and dangerous.”
Considering the amount of treatment and therapy in progress, Kopelan said, he’s unsure whether he’d be willing to take the same risk today. “When Rafi was born in 2007, there was no biotechnology or pharmaceutical work being done for EB patients. Now, 10 companies are pursuing.”
Still, he said the bone marrow transplant procedure has changed dramatically over the years. In particular, an experimental treatment led by the University of Minnesota is truly groundbreaking. “The procedure overall is safer, there aren’t as many side effects, and it’s potentially more effective,” he said.
Advancements are surely needed, Kopeland said, because the quality of life for many EB patients is often very low. “You have to keep wounds clean, and there’s a constant risk of life-threatening infection,” he said. “You know how you get a paper cut and put Purell on it and it stings? Imagine if you had this over 60 percent of your body. You’re in a constant state of pain with very little relief.”
Each morning, the Kopelans go through a 90-minute ritual of wound care and prevention, followed by a two-hour after-school routine with their only child. Rafaella uses methadone for pain and a gastrointestinal tube for most of her caloric intake. Every four months or so she has her esophagus dilated. Then there are trips to Cincinnati Children’s Hospital Medical Center, where she sees a host of specialists.
“The daily routines are arduous, painful, anxiety-producing,” Kopelan said. “Just going to the bathroom is painful. My daughter wakes up scared every morning that her PJs are stuck to her.”
Still, he said that Rafaella, like most children with EB, does all she can to live a normal life. When she isn’t speaking to large groups globally about the disease, she loves playing with her dog and singing, drawing and painting. Although accompanied by a nurse to help with bathroom visits, Rafaella attends a regular school.
“The kid’s got a great spirit,” Kopelan said. “And she’s got really great friends.”