Epidermolysis bullosa causes
Epidermolysis bullosa (EB) comprises a group of rare skin blistering disorders that cause the skin and mucous membranes lining parts of the body to become extremely fragile and prone to blistering and tearing, even with minor friction.
The skin is organized into several layers. Two of the most important are the epidermis, or outermost layer, and the dermis, the supporting layer underneath. They are held together by a specialized structure called the basement membrane. The ability of these layers to remain physically linked is essential to the skin’s integrity and function.
EB arises when one of the structural proteins needed for these connections within or between skin layers is missing, reduced, or not functioning properly. This usually happens due to mutations in genes that provide instructions for making these proteins. Identifying the genetic causes of EB is essential to diagnose the condition, guide treatment, set long-term expectations, and support family planning decisions.
The role of genes in EB
Mutations in at least 18 genes that encode key structural proteins in the skin have been linked to EB. The specific gene and type of mutation influence disease severity and which layer of the skin is affected.
EB gene mutations can be:
- inherited, or passed down from biological parents
- spontaneous, meaning they occur randomly in a person with no EB family history
While these mutations may lead to similar symptoms, they differ in terms of risk and the likelihood of passing the disease to future generations.
Inherited vs. spontaneous genetic mutations
EB is typically caused by mutations in genes found on non-sex chromosomes. Most people carry two copies of each of these genes, one inherited from each biological parent.
EB can be passed down in different ways, and is typically classified based on its inheritance pattern:
- Autosomal dominant: A single faulty gene copy inherited from one parent with EB is enough to cause the disease. Each child has a 50% chance of inheriting and developing the condition.
- Autosomal recessive: Two faulty gene copies from both parents, who each carry a mutated copy of the gene, are needed for the disease to develop. Each child has a 25% chance of inheriting both mutations and developing the disease.
In some cases, there is no hereditary component, and EB is caused by spontaneous, or de novo, mutations that arise randomly before birth in a person with no family history of the disease. In this situation, the chances of two healthy parents having more children with EB due to a spontaneous mutation are very low. Still, a person with an EB spontaneous mutation has a 50% chance of passing it on to their biological children.
How different types of EB develop
There are more than 30 genetic subtypes of EB grouped into four main types, based on the layer of the skin affected and the genes and proteins involved:
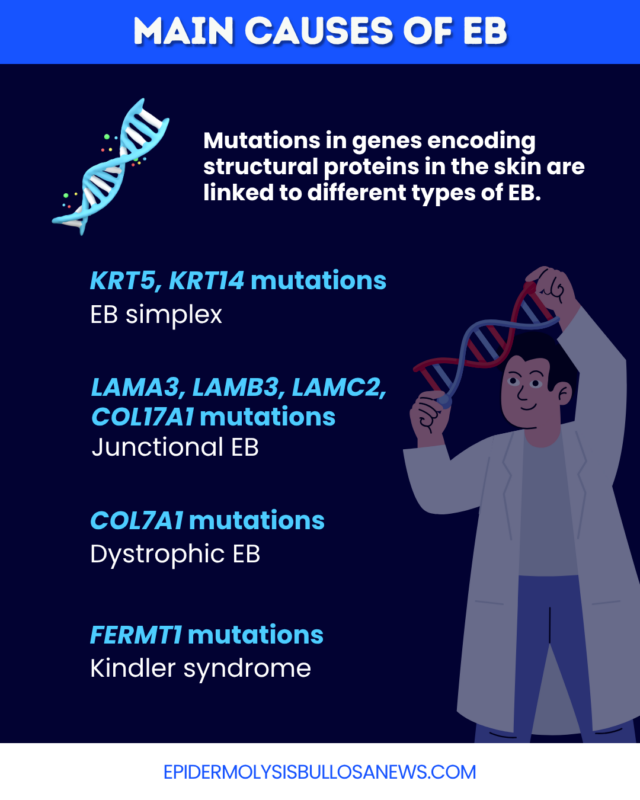
- EB simplex (EBS): Caused by mutations in genes encoding keratins and other proteins needed for the integrity of the epidermis, including KRT5 and KRT14. It is usually inherited in an autosomal dominant manner and causes blisters to form in the epidermis.
- Junctional EB (JEB): Caused by mutations in genes encoding part of laminin-332 and other proteins that help anchor the upper and lower layers of the skin, including LAMA3, LAMB3, LAMC2, and COL17A1. It is inherited in an autosomal recessive manner and causes blisters to form in the basement membrane.
- Dystrophic EB (DEB): Caused by mutations in the COL7A1 gene, which encodes a protein needed to assemble a larger protein called type VII collagen that plays a key role in anchoring skin layers. It can be inherited in an autosomal dominant or recessive manner and causes blisters to form in the dermis.
- Kindler syndrome: Caused by mutations in the FERMT1 gene, which encodes a protein called kindlin-1 that plays a key role in skin integrity. It is inherited in an autosomal recessive manner and causes blisters to form across the different skin layers.
Besides these genetic forms of EB, there is also a rare autoimmune disease that causes similar symptoms called EB acquisita (EBA). In EBA, the immune system mistakenly produces antibodies that target type VII collagen, leading to symptoms similar to those of DEB. The exact reasons why this happens are not fully understood.
When do symptoms usually begin?
EB typically presents at birth or in early childhood. It may become more noticeable as a child grows and begins to crawl or experience friction from diapers and clothing. In milder cases, symptoms may not appear until later childhood, adolescence, or even early adulthood.
Unlike genetic forms of EB, EBA typically develops in adulthood, often after the age of 40.
The onset and severity of EB can vary depending on several factors, including:
- the specific disease subtype and type
- the nature of the genetic mutation and how it affects protein production or function
- inheritance pattern
- a person’s activity and overall health
- access to treatment and care
Next steps after learning the cause
A diagnosis of EB typically begins with the recognition of early symptoms, reviewing a person’s family history, and ruling out other possible causes.
Additional tests may then be used to confirm the diagnosis and determine the disease’s type and subtype. These tests are important for guiding medical treatment and informing family planning:
- Genetic testing: DNA from blood or cheek swabs is analyzed to identify known EB-causing mutations. This is generally considered the gold standard test for diagnosing EB and determining its type and subtype.
- Skin biopsy and microscopy: A small skin sample is removed and examined under a microscope. This test can help evaluate skin structure and identify missing or abnormal proteins, helping determine the disease’s type and subtype.
After receiving an EB diagnosis and understanding its cause, patients should work with a multidisciplinary team of specialists to develop a treatment plan tailored to their needs. Connecting with national and international support organizations, such as DEBRA of America and DEBRA International, which offer education, emotional, and practical support, can also help improve quality of life for patients, families, and caregivers.
Can EB be prevented?
Genetic forms of EB do not have a cure and cannot be prevented through lifestyle, behavioral, or environmental changes. Genetic screening can help determine whether parents are EB carriers. With guidance from a genetic counselor, parents can assess the risk of passing on the disease before deciding to have children and consider steps to reduce the risk, including:
- choosing not to have biological children if they are found to be EB carriers
- using preimplantation genetic testing, which allows embryos to be screened for specific EB mutations before being implanted in the womb during in vitro fertilization
- opting for prenatal testing to determine whether a developing fetus has EB
EBA also cannot be prevented, because its exact causes are not fully understood.
Epidermolysis Bullosa News is strictly a news and information website about the disease. It does not provide medical advice, diagnosis, or treatment. This content is not intended to be a substitute for professional medical advice, diagnosis, or treatment. Always seek the advice of your physician or other qualified health provider with any questions you may have regarding a medical condition. Never disregard professional medical advice or delay in seeking it because of something you have read on this website.
 Fact-checked by
Fact-checked by 

