Choosing Between Bad and Worse, I Learned to Become an Advocate
Written by |
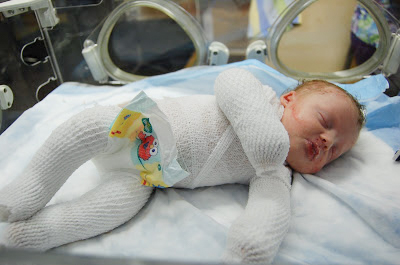
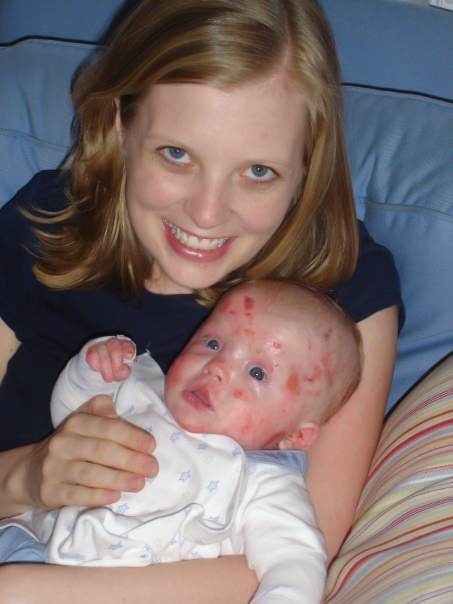
(Courtesy of Patrice Williams)
The scariest thing about a rare disease is that nobody has the answers you’re desperately seeking. When you are facing something so unfamiliar and the people who are supposed to know don’t, it’s terrifying.
The first couple months of the life of my son Jonah, who was born with epidermolysis bullosa (EB), felt like complete guesswork. The only choices we had were either bad or worse, and we had to choose between two horrible options.
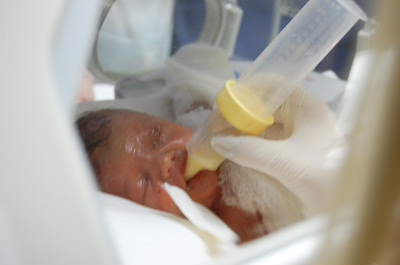
Jonah couldn’t eat because of blisters in his mouth and esophagus. Any bottle we tried caused blistering. We couldn’t use tape to secure a nasogastric feeding tube, so the tube would slip up to his throat and start choking him.
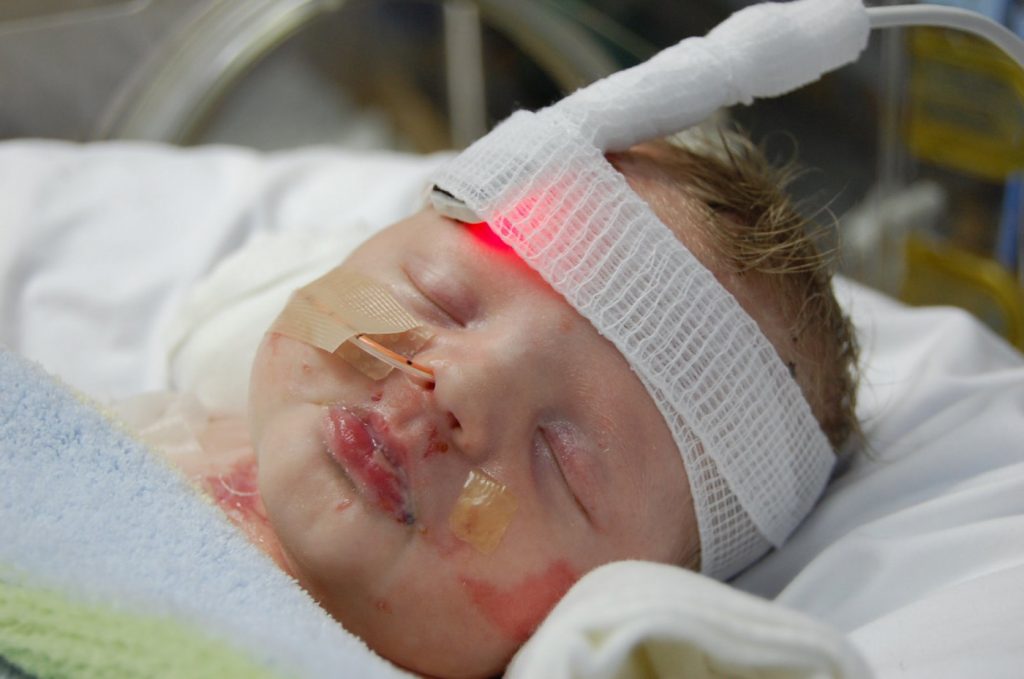
We couldn’t give him strong pain meds because we couldn’t monitor his oxygen because we couldn’t figure out how to attach a pulse oximeter without ripping his skin. After he stopped breathing on day two because of high doses of fentanyl, I was terrified that he wasn’t on an alarm.
We couldn’t run antibiotics via IV because we didn’t know how to safely secure one. Every IV we tried came out and took skin in the process.
We couldn’t bandage him in the correct EB-safe bandages because at first, we didn’t even know they existed. When we did, the hospital didn’t have them on hand.
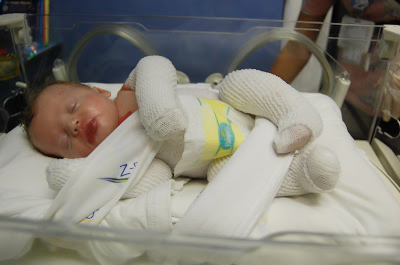
He couldn’t wear a regular diaper because the elastic blistered his legs. We tried cloth diapers, but they wouldn’t absorb because of all the Aquaphor we had to slather all over him. If urine leaked out, we had to redo his leg bandages.
The list went on and on.
My breaking point was one night, after days of not eating, the doctors were going to try a central line near Jonah’s neck. He had to have nutrition, but I knew the line would tear his skin to pieces and probably wouldn’t stay anyway. And if it didn’t work, it meant G-tube surgery, which would require intubation, a dangerous scenario for EB babies.
I was completely at the end of myself. I cried and screamed — literally screamed — at God all the way home. Something had to give. I couldn’t handle the stress of choosing between the bad or the even worse.
The doctor called me that night at 3 a.m. after trying the procedure. “We couldn’t do it, Patrice,” he said. “It wouldn’t stay, and we ripped a big patch of skin.”
“OK,” I said simply. God had given me peace, and I wasn’t so afraid anymore. I knew we were going to figure it out. I turned back over and went right to sleep.
The next day, Jonah started eating — not a lot, but enough to avoid intubation and surgery. I also went to the doctors and asked for help. Jonah was at an amazing teaching hospital, but his doctor was changing every week, and they kept assigning different nurses to his care. It was not ideal.
With such a rare diagnosis, I was exhausted from explaining and reexplaining. “You can’t use tape.” “This is how we have to do the pulse ox.” “No, you can’t pick him up like that.” “This is how we have to bandage.”
In response to my pleas, the doctors created a primary care team. Jonah had one on-call doctor that would help me make all the decisions, and he had the same team of nurses on each shift. Although they didn’t know the answers, his team was willing to do whatever it took to find them. And I was the primary person on that team.
At rounds each day, I would ask a million questions and document each answer. “Could you repeat that?” “What was that called again?” “Can you explain what that means?” The doctors were so patient, and the nurses were my biggest cheerleaders.
I gave daily updates about Jonah on our blog, and EB caregivers and patients would reach out in the comments with things to try. My sister-in-law compiled the suggestions into documents for me to take to his medical team. And they would accept my input with eagerness and open minds.
Since then, advocating for Jonah has become second nature. I have learned to speak up and to trust my instincts. I’ve sought out doctors who will think outside the box. I’ve realized that I may not know all there is to know about epidermolysis bullosa, but I know my kid.
You are your own biggest advocate. When something doesn’t feel right, speak up. Find a medical team that values your input and holds you in high regard.
Never stop fighting for yourself. You don’t know all there is to know about the disease, but you need to be the starting player surrounded by a solid team willing to do what it takes to figure it out. They do exist. And they’re worth fighting for.
***
Note: Epidermolysis Bullosa Today is strictly a news and information website about the disease. It does not provide medical advice, diagnosis, or treatment. This content is not intended to be a substitute for professional medical advice, diagnosis, or treatment. Always seek the advice of your physician or other qualified health provider with any questions you may have regarding a medical condition. Never disregard professional medical advice or delay in seeking it because of something you have read on this website. The opinions expressed in this column are not those of Epidermolysis Bullosa Today or its parent company, Bionews, and are intended to spark discussion about issues pertaining to epidermolysis bullosa.



Leave a comment
Fill in the required fields to post. Your email address will not be published.