Fighting for Insurance to Cover My Son’s Lifesaving Bandages
Written by |

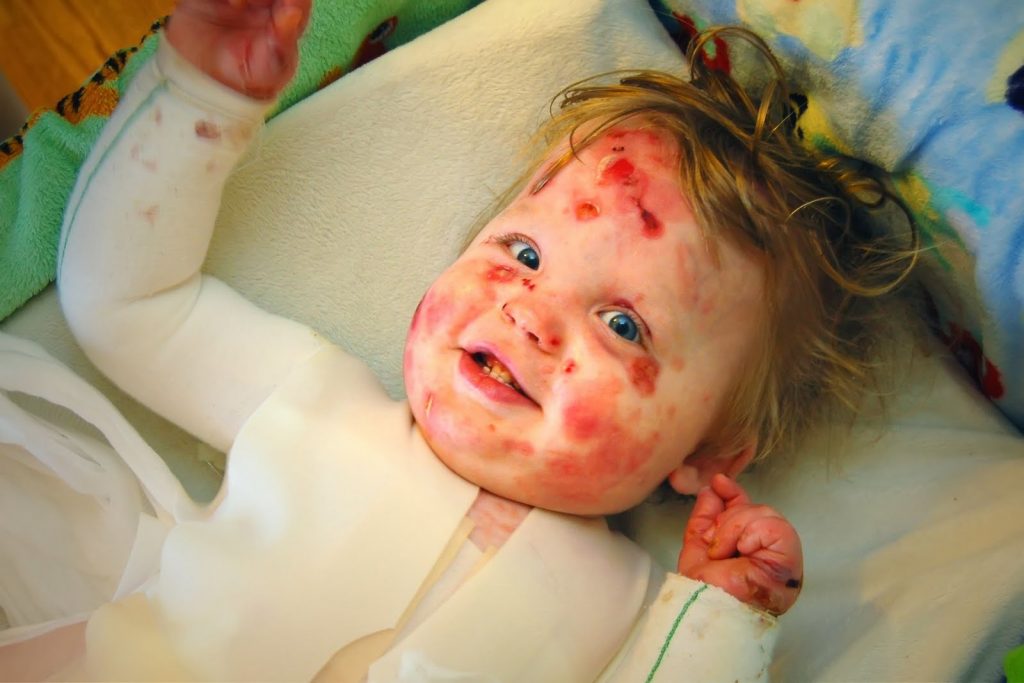
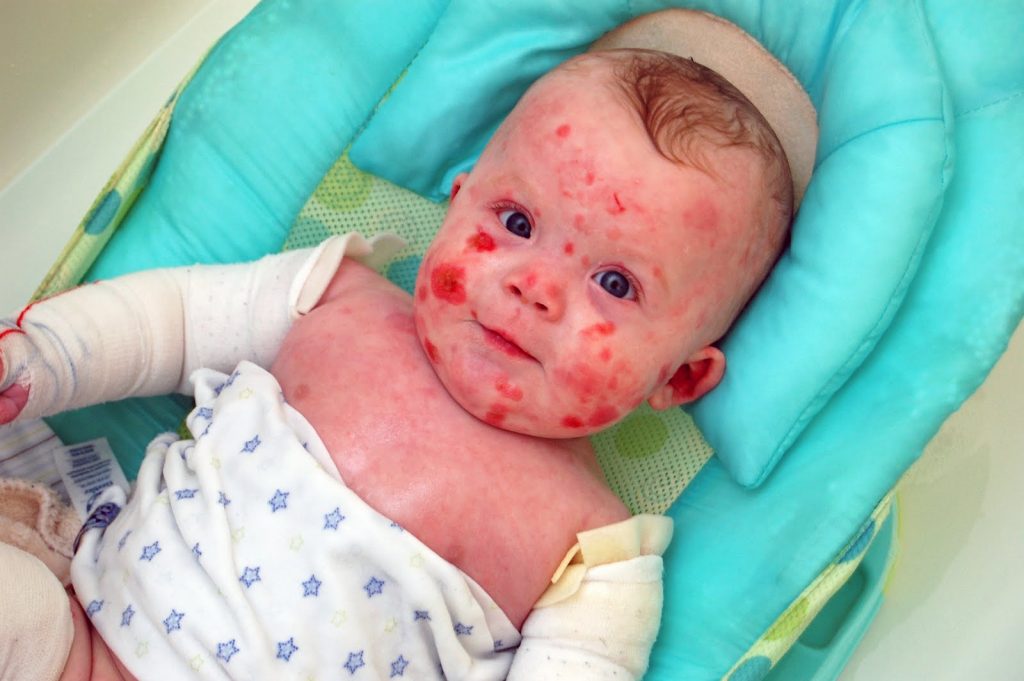
Jonah, my 11-year-old son who has epidermolysis bullosa (EB), is wounded from head to toe and must be covered in lifesaving bandages every single day. These bandages not only cover his current wounds, prevent infection, and promote healing, but also give him a layer of “skin” that keeps him from developing innumerable, all-encompassing wounds. We partially change his bandages every day, and fully change them every other day.
As he gets bigger, more bandages are required. We use a bottom contact layer that prevents sticking, a waterproof layer that we cut down to patches to cover individual wounds, a large nonstick sheet layer that goes on top of that, a gauze roll layer to keep it all secure, and finally, a sleeve layer on top.
With three to four full-body bandage changes a week, plus in-between touch-up care, the out-of-pocket cost to save Jonah’s life would be more than $12,000 a month. A month. A friend and I recently totaled up his bandage costs, and if we were paying out of pocket, each dressing change would cost a minimum of $900. Thank God for insurance.
Except not really. Because most insurance companies, including ours, don’t cover bandages. It doesn’t matter that they are needed for these kids’ survival. It doesn’t matter that they are medically necessary. It doesn’t matter that people with EB would literally die without them. They are not covered. (And no amount of tears will change their minds, I can tell you that firsthand.)
No worries. There’s always Medicaid. Or is there? Only six of 50 states have Medicaid programs that cover the bandages that people with epidermolysis bullosa desperately need.
Recently, we had friends who had to uproot their entire lives because their insurance switched and no longer covered bandages. Nor did New York Medicaid. Our friends had the resources and the means to move to Colorado, where Medicaid will cover their daughter’s supplies. But many others are not so fortunate.
Even with their ability and resources to move, they’ve given up their friends, family, and entire support network to move across the country. Now, their young teenage daughter is faced with having to make new friends, a feat made even more difficult with an isolating disorder like EB.
But what choice did they have?
We had a scare about two years ago when my husband’s company changed insurance providers. The new provider said “no way” to covering bandages, and North Carolina Medicaid was denying us as well. After a month of sheer panic, and some people in very high places getting involved, we were finally able to find a bandage company and Medicaid codes that covered Jonah.
The EB community, being what it is, would never have let him go without, but donated bandages would have been a very short-term solution. The cost on other families would have been too great, and we certainly couldn’t have paid 10 times the amount of our mortgage, per month, to purchase the EB-safe bandages out of pocket.
Ten times the amount of our mortgage.
I’m no politician, and I will not pretend to know the ins and outs of privatized health insurance, Medicaid, Medicare, or universal healthcare. But people should never be put in this kind of situation. You should never be just one diagnosis away from destitution. Forget about the unalienable rights to liberty and the pursuit of happiness. Can we back up to the right to life?
Why can insurance companies deny lifesaving treatments that are, without a doubt, medically necessary? Why don’t all states have consistent Medicare and Medicaid coverage that will cover these supplies? Why are patients and families who already deal with the pain, suffering, and hopelessness of EB forced to also live in fear of insurance changes or loss of coverage when their very lives depend on it?
To me, it comes down to basic human decency. I don’t have the answers, but more folks need to be aware of this issue. And I believe it’s something worth fighting for.
***
Note: Epidermolysis Bullosa Today is strictly a news and information website about the disease. It does not provide medical advice, diagnosis, or treatment. This content is not intended to be a substitute for professional medical advice, diagnosis, or treatment. Always seek the advice of your physician or other qualified health provider with any questions you may have regarding a medical condition. Never disregard professional medical advice or delay in seeking it because of something you have read on this website. The opinions expressed in this column are not those of Epidermolysis Bullosa Today or its parent company, Bionews, and are intended to spark discussion about issues pertaining to epidermolysis bullosa.




Leo Ducharme
I am with you 100%, as a eb patient myself I am constantly fighting with the insurance company and suppliers about receiving bandages. They fight you over which ones you can get, the amount you can receive, and amount per wound- no matter the size. I have been fighting this battle for years, but it seems lately it is becoming extremely difficult to get what you need.